“It was the best of times, it was the worst of times,” says every organization after an EHR go-live.
I’ve had the great opportunity to meet with a number of dedicated professionals that continually strive to align their health systems with the Quadruple Aim:
- Improving health of the population
- Improving patient experiences
- Reducing costs of care
- Improving clinician work life
Among the stakeholders that I connect with, an inevitable delineation is between the efforts that fall within clinical informatics and those that sit more squarely within quality improvement teams. This differentiation is typically defined by reporting structures and, ultimately, funding sources.
However, in the domain of clinical decision support (CDS), I’ve been a strong advocate of viewing the responsibility for areas of impact as belonging to a continuum rather than belonging to a well delineated set of groups. After all, the clinical informatics teams aren’t building electronic interventions just to check a box. At the same time, quality teams shouldn’t be requesting help with electronic interventions if nobody knows if they are working. Given the varied reporting structures, who takes responsibility for what?
Operationalizing CDS
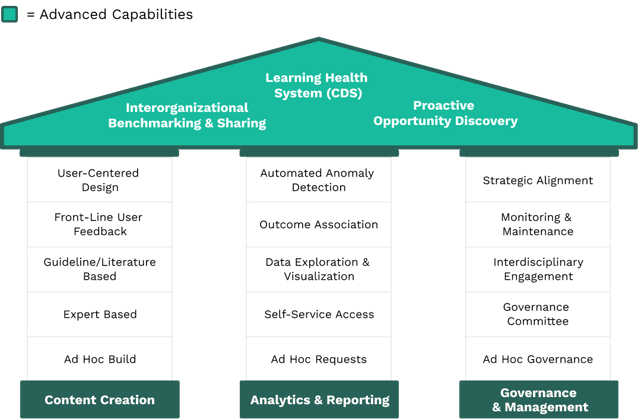
Along with some colleagues, Phrase published a CDS maturity model based on interviews conducted with close to a hundred informatics and quality-oriented professionals. The findings reflect an evolution that health systems step through as they improve their approach to optimizing the electronic health record (EHR) system.
To summarize, there are fundamentally three foundational domains:
- Content creation
- Analytics and reporting
- Governance and management
All three of these domains require close collaboration and coordination between clinician informatics and quality improvement teams. For example, when constructing a sepsis alert, the clinical informatics team must work closely with the quality team to understand what the alert content should consist of to ensure it’s aligned with other interventions and the desired outcomes. Additionally, the informatics team may need to build in a discrete reporting field to help facilitate downstream impact, but that is only known if the downstream measure has been defined by the quality team.
Who owns the output of electronic workflows?
Traditionally, the clinical informatics team takes the lead on these CDS “experiments.” This includes vetting new requests from across the health system, assisting IT teams with implementation around variable workflows, and fielding complaints regarding the multitude of existing interventions. This is a monumental task and, not surprisingly, smaller clinical informatics teams don’t have bandwidth to accomplish all this while also monitoring the thousands of CDS “experiments” that are ongoing. Quality teams, on the other hand, monitor outcomes and orchestrate their initiatives across electronic domains, but also importantly: outside of the EHR.
This is where the chasm exists between the siloed clinical informatics and quality teams. I’ve seen some health systems take the step of requiring 1- and 6-month reports from the requestor after a new CDS implementation. If the CDS isn’t moving the needle (or the requestor fails to report back), the CDS is removed. This is a draconian approach, but represents a forceful attempt to integrate these silos. A softer approach uses the intake process itself to encourage alignment. As part of some intake forms, the clinical informatics team asks questions like: “what process measure is this intended to drive?” and “who will be responsible for monitoring this CDS intervention?”
As a side note, we collected the intake forms and processes from over 20 health systems. Feel free to reach out to me if you’d like a copy of these anonymized forms and associated description of their processes.
Bringing it together
When it comes to improving outcomes via the EHR, clinical informatics and quality improvement teams must be closely integrated. This starts with an integrated governance structure where quality improvement teams co-lead and attend CDS meetings with the informatics teams. With assistance from clinical informatics, the quality teams must apply their PDSA approach to electronic workflows and request modifications (or removal) when these interventions are not meeting goals.
One way to ease efforts of integration is embracing technology. Phrase Health helps informatics teams juggle the electronic workflow library and connects quality improvement teams back to these interventions. However it's accomplished, bridging these silos is necessary for health systems to more efficiently and reliably meet desired outcomes.
Check out more content
Next: Partnering to Conquer Complex Problems
Previous: Mission Impossible: Harnessing the Power of the EHR

